The biggest “Ozempic surprise” isn’t on the scale—it’s that a drug celebrated for metabolic progress can expose a literal blind spot in eye health.
Quick Take
- GLP-1 drugs like Ozempic and Wegovy can deliver major weight and blood-sugar wins, but rapid glucose shifts can briefly blur vision and may aggravate existing retinal disease.
- Research has raised concern about rare, sudden vision-loss conditions such as non-arteritic anterior ischemic optic neuropathy (NAION) and other ischemic optic neuropathies (ION), with dose possibly influencing risk.
- Absolute risk signals in newer studies appear low, yet the stakes feel high because optic nerve injuries can be irreversible.
- The most practical takeaway: people with diabetes or known retinopathy should treat eye monitoring as part of “metabolic health,” not an optional add-on.
When a “Metabolic Fix” Moves Faster Than Your Eyes Can Handle
Semaglutide didn’t become a household name because it promised better eye charts. It became famous because it reliably lowers blood sugar and helps many patients lose weight—two outcomes tied to longer life and fewer complications. The trouble starts when success happens quickly. Rapid drops in glucose can temporarily change the eye’s lens shape and hydration, leaving some patients with blurred vision that feels sudden and alarming.
That blur often improves as glucose stabilizes, but the episode serves as a warning light: the eye is a metabolically sensitive organ fed by delicate blood vessels. People over 40 already know how unforgiving vision changes can be. Add diabetes, hypertension, sleep apnea, or high cholesterol—common companions of obesity—and you have a population where small vascular disruptions can carry outsized consequences.
The Retinopathy Problem: Old Diabetes History, New GLP-1 Timing
Worsening diabetic retinopathy after rapid glucose improvement isn’t a new phenomenon; diabetes research has documented “early worsening” when control tightens quickly. GLP-1 medications can accelerate that timeline by improving glucose and sometimes lowering appetite dramatically, changing what and how people eat. For patients with pre-existing retinopathy, that speed matters.
Dry eyes and irritation also show up in real-world complaints, and they can feel trivial until they become constant. In drier climates or during heavy screen time, symptoms can pile up. The practical point isn’t that GLP-1 drugs “cause” every eye nuisance; it’s that people starting these drugs often change hydration, diet, and body chemistry at once. When the body shifts quickly, the surface of the eye can become one more place where strain shows.
NAION and ION: The Rare Event That Changed the Conversation
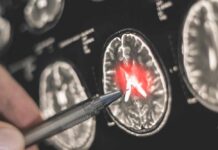
The phrase “Ozempic blindness” took off online because it compresses a frightening scenario into two words: sudden vision loss. The conditions at the center of that fear—NAION and related ischemic optic neuropathies—are typically vascular events affecting the optic nerve, often described as a “stroke of the optic nerve.” A matched-cohort study in a major ophthalmology journal helped quantify a signal that demanded attention.
Later reporting and analyses layered on nuance: risk appears rare in absolute terms, yet certain comparisons have suggested differences by formulation and dose. Wegovy, commonly used at a higher dose for weight loss than Ozempic’s typical diabetes dosing, has drawn scrutiny after findings that pointed to higher odds of ischemic optic neuropathy. A dose-response pattern, if confirmed, would fit basic pharmacology and basic logic: more drug can mean stronger effects—and potentially stronger side effects.
Confounding Factors: The Boring Detail That Determines What’s True
Eye researchers and clinicians keep returning to the same uncomfortable reality: people prescribed GLP-1 drugs often already carry the very risk factors that can lead to optic nerve ischemia. Diabetes and obesity correlate with vascular disease. Hypertension and sleep apnea don’t help. That doesn’t “clear” the medication, but it does complicate clean cause-and-effect claims. Retrospective datasets can flag associations without proving the drug pulled the trigger.
That said, dismissing signals because they’re inconvenient violates common sense too. When millions of Americans use a medication, even a small increase in a rare outcome becomes a real number of affected people. The adult, responsible approach sits in the middle: treat the evidence seriously, avoid hysteria, and insist on better prospective research while using today’s knowledge to reduce preventable harm.
What Patients Should Do Now: A Checklist Mentality, Not a Scare Campaign
People considering semaglutide should stop thinking of “metabolic health” as labs and waist size only. Vision deserves a seat at the table, especially for anyone with diabetes, known retinopathy, prior eye injections or laser treatments, or episodes of unexplained vision loss. Baseline eye exams and follow-ups create a paper trail and a clinical trail. They also protect patients from delayed diagnoses that get blamed on the wrong thing.
Symptoms should drive urgency. Sudden blind spots, a curtain-like shadow, new floaters with flashes, or abrupt vision loss merit immediate evaluation. This isn’t political; it’s practical. People do not get a second chance with optic nerve tissue. If a clinician suggests slower titration or closer glucose monitoring to avoid sharp swings, that advice aligns with the core lesson here: steady improvement beats dramatic whiplash when organs rely on micro-blood flow.
GLP-1 drugs remain valuable tools, and the Cleveland Clinic view that benefits often outweigh risks for many diabetics reflects the broader medical consensus. The honest bottom line is still unsettling: the same medications that help Americans reclaim health can also expose vulnerabilities in the eyes, especially when used aggressively or without baseline screening. The “blind spot” isn’t the drug—it’s the habit of treating eyesight as separate from metabolism.
Sources:
How Medications Like Ozempic Affect Your Vision
Can Semaglutide Cause Eye Problems?
Wegovy users may have 5 times the risk of vision loss vs Ozempic, study suggests
GLP-1 Drugs and the Risk of Losing Vision
Ozempic and Blindness: Is There a Link?
Scientists Explain ‘Ozempic Blindness’: Link Between Sudden Vision Loss and Weight Loss Drugs
GLP-1 drugs tied to low but elevated risk of age-related macular degeneration
Risk of Nonarteritic Anterior Ischemic Optic Neuropathy in Patients Prescribed Semaglutide